Pokémon Go: Exercise or Video Game?
By now I am sure that you have heard about – and probably even seen people playing – the wildly popular new app, Pokémon Go. With tens of millions of downloads in the US alone, the app is reportedly earning $5 million per day, and that is just on micro transactions (in-app purchases). Not bad, for a free app. Read More
Breeding Bravery
The word “brave” has many synonyms. Courageous. Valiant. Heroic. But what does it really mean to be brave? And more importantly, how do we create bravery in ourselves and in our children?
Independent vs. Self-Sufficient
We have all heard kids say it. No, demand it! “I WANT TO DO IT!”
The ultimate goal of parenting is to help our children become competent, productive, and happy adults. This 18+ year process is never easy, but as children develop and attempt to explore the range of their own abilities, parents often find themselves trying to strike a balance between allowing their kids to be independent and making sure that everything gets done in the best, most efficient manner. Read More
Another Mass Shooting
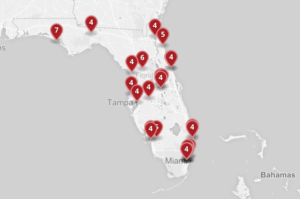
Florida Mass Shootings in 2015
from PBS (http://www.pbs.org/newshour/rundown/heres-a-map-of-all-the-mass-shootings-in-2015/)
Having lived in the central Florida area my entire life, we have certainly had our share of violent acts. According to an Orlando Weekly blog post from December 2015, there were 27 mass shootings in Florida in 2015 (read the blog post here). What’s more, according to the website shootingtracker.com, there have already been 14 mass shootings in Florida for 2016. These figures exclude the mass shooting from this past weekend, where – according to information available at the time of this writing – 20 people were killed and 42 were injured. Read More
Getting Ready for S.U.M.M.E.R.
As Alice Cooper heralded, “School’s out for summer!” Students are more than ready to be out of class and away from school for the next few months. And let’s be honest, most parents are eager for the end of the school year as well. No more homework battles. No more projects. No more teacher conferences. Read More
Now Available: The Handbook for Raising an Emotionally Healthy Child Part 1
It has been a few days since I have written a post because we have been busily working to get everything organized and prepared for today, the launch of our new Kindle book, The Handbook for Raising an Emotionally Healthy Child Part 1: Behavior Modification. Read More
Who’s Responsibility is it to Learn?
For most of us, the past two months have been filled to the brim with stress. Students have been testing away, on state and district mandated tests. Teachers are hurriedly trying to squeeze everything into the next few weeks. The end of the school year must certainly be approaching. Read More
Resource 7: Balancing Control and Reactivity
As I mentioned in Wednesday’s blog, the past few weeks have been dedicated to performing the final review and edits to Part One of the revised Handbook for Raising an Emotionally Healthy Child, which will be available as a Kindle e-book on May 9, 2016. The revisions are really coming together very well and we believe that the information will help parents find more joy and pleasure in their task of being a parent. Read More
Raising an Emotionally Healthy Child – Part One
It has been a while since I offered an update on some of the things we have in the works. So I thought I would take the opportunity in this mid-week post to catch you up a bit. Read More
Self-Harming Behaviors and Teenagers
Self-harming behaviors have garnered a great deal of attention over the past few years. While the prevalence of intentional self-harm – the most common of which include cutting and burning – continue to rise, it is difficult to truly understand the rationale for these behaviors. Nonetheless, it has become somewhat of an “en vogue” coping strategy many teenagers are using to deal with depression and heightened emotionality.
Cutting has reached the mainstream media. Read More






